The global obesity epidemic continues to pose a significant health challenge. Shockingly, recent data from health authorities reveal that over 30% of adults in the United States struggle with obesity. While the first line of defense typically involves dietary changes and exercise, the reality is that many individuals find it challenging to shed excess weight through these methods alone. That’s where bariatric surgery is a game-changer for those in need. But here’s the catch: not everyone qualifies for surgery, leaving many individuals with Type I obesity or BMIs ranging from 25 to 35 kg/m² searching for effective alternatives. As a result, there’s a growing interest in minimally invasive weight loss procedures. These procedures offer a potentially less drastic alternative to traditional bariatric surgeries, with shorter recovery times and less surgical risk.
One emerging option within these possibilities is gastric BOTOX®. This endoscopic procedure involves injecting botulinum toxin (BOTOX®) into the stomach wall as a means to promote weight loss in carefully selected patients. By understanding how gastric BOTOX® works, we can explore its potential role in the evolving techniques of obesity management.
What Does BOTOX® in the Stomach Do?
BTX is initially synthesized as an inactive single-chain polypeptide with a molecular weight of around 150 kDa. This chain undergoes cleavage into a heavy chain (approximately 100 kDa) that binds to presynaptic cholinergic nerve terminals and a light chain (around 50 kDa) responsible for inhibiting neurotransmitter release. Each toxin subtype has a distinct structure.
The factors that make BOTOX® stomach injections an interesting alternative to other weight loss modalities include:
- Reversibility: Unlike some bariatric surgeries, gastric BOTOX®’s effects wear off over time. This can be appealing to some people who may not want a permanent alteration to their digestive system.
- Potential for specific patient groups: Gastric BOTOX® might be an option for individuals with a body mass index (BMI) that doesn’t qualify them for traditional bariatric surgery or for those considered high-risk surgical candidates due to underlying health conditions.
- Nerve-blocking properties of botulinum toxin A (BTX-A) might be harnessed within the stomach wall. This approach could induce sensations of fullness, slow down the rate of gastric emptying, and promote earlier feelings of satiety, potentially leading to weight loss. This method shows promise with fewer complications than others.
Mechanism of Action
- Target: BTX A specifically targets the neuromuscular junction (NMJ)
- Binding: It binds to specific receptors on presynaptic nerve terminals.
- Internalization: BTX A enters the cell via endocytosis (estimated internalization rate: 1-2 hours).
- SNARE Complex Disruption: Inside the cell, the light chain cleaves proteins within the SNARE complex, particularly SNAP-25, thereby inhibiting ACh release.
- Neuromuscular Transmission Block disrupts neuromuscular transmission, leading to temporary, localized chemical denervation and muscle weakness.
Duration of Effect
BTX A’s effects are temporary due to nerve regrowth and new receptor formation. This typically takes 4-6 weeks for full return of function. Ongoing research aims to extend the duration of BTX by targeting regenerative mechanisms. This could mean adding an extra 2-4 weeks of effectiveness.
Who May Benefit from Gastric BOTOX® Procedure?
Prior to performing the ‘tummy BOTOX®,’ careful patient selection and evaluation by a healthcare professional are crucial. Here’s a breakdown of who might be a good candidate:
- Moderate Weight Loss Goals: Adults seeking to lose weight for specific purposes, such as before elective surgery or to improve fertility outcomes.
- Body Mass Index (BMI): Generally, patients with a BMI between 30 and 40 (considered obese) who haven’t achieved significant weight loss with diet and exercise alone.
- Limited Success with Lifestyle Changes: Individuals who have struggled to lose weight despite implementing lifestyle modifications like diet and exercise may benefit from the additional support offered by gastric BOTOX® procedure.
- Individuals Tackling Lifestyle Disorders: By promoting weight loss, gastric BOTOX® can potentially reduce the risk of developing weight-related health problems like high blood pressure, diabetes, stroke, sleep apnea, and heart disease.
Important Considerations:
- The absence of major medical conditions that could complicate the procedure or compromise safety (e.g., severe gastroparesis, history of bowel obstructions).
- Setting unrealistic expectations can lead to disappointment. It’s essential for patients to understand that gastric BOTOX® is a tool to support weight management, not a quick fix.
- Patients who understand and accept the potential side effects and limitations of gastric BOTOX® are well-positioned for informed decision-making.
Gastric BOTOX® in Obesity: A Look at Current Research
When it comes to BOTOX® injections in stomach for weight loss, current research paints a complex picture, suggesting it may not be a one-size-fits-all solution. Initial investigations into Botulinum Toxin A (BTX) for weight management yielded mixed results. While animal studies were encouraging and showed promising weight loss results, human trials were inconsistent.
Larger RCTs offered some clarity but revealed a crucial factor: injection location. Targeting the antrum or angulus (lower stomach) alone showed no substantial weight loss compared to placebo. However, studies injecting both the antrum and fundus (upper stomach) demonstrated promise. Notably, one RCT using this combined approach achieved an average 11 kg weight loss in morbidly obese patients.
Despite promising results, challenges persist. Limited studies, methodological variations, and the absence of standardized protocols regarding injection sites and dosage create uncertainties about BTX’s long-term effectiveness for weight loss.

BOTOX® in Gastrointestinal Disorders: A Safer Alternative?
Beyond its potential for weight management, BOTOX® is a minimally invasive option for those with advanced esophageal disorders who can’t tolerate or prefer to avoid other procedures. Although its efficiency in treating various gastrointestinal disorders can vary, BOTOX® has shown promising results in treating certain conditions.
For example, injecting BOTOX® in the stomach for gastroparesis has shown positive effects by relaxing the pyloric sphincter and improving gastric emptying. However, the evidence still needs to be conclusive, and larger, well-designed trials are needed to determine the overall efficacy.
It is important to note that while BOTOX® shows potential in treating some gastrointestinal disorders, it is not a cure-all treatment. Each patient’s response to BOTOX® may differ, and other treatment options should also be considered based on individual circumstances and medical advice.
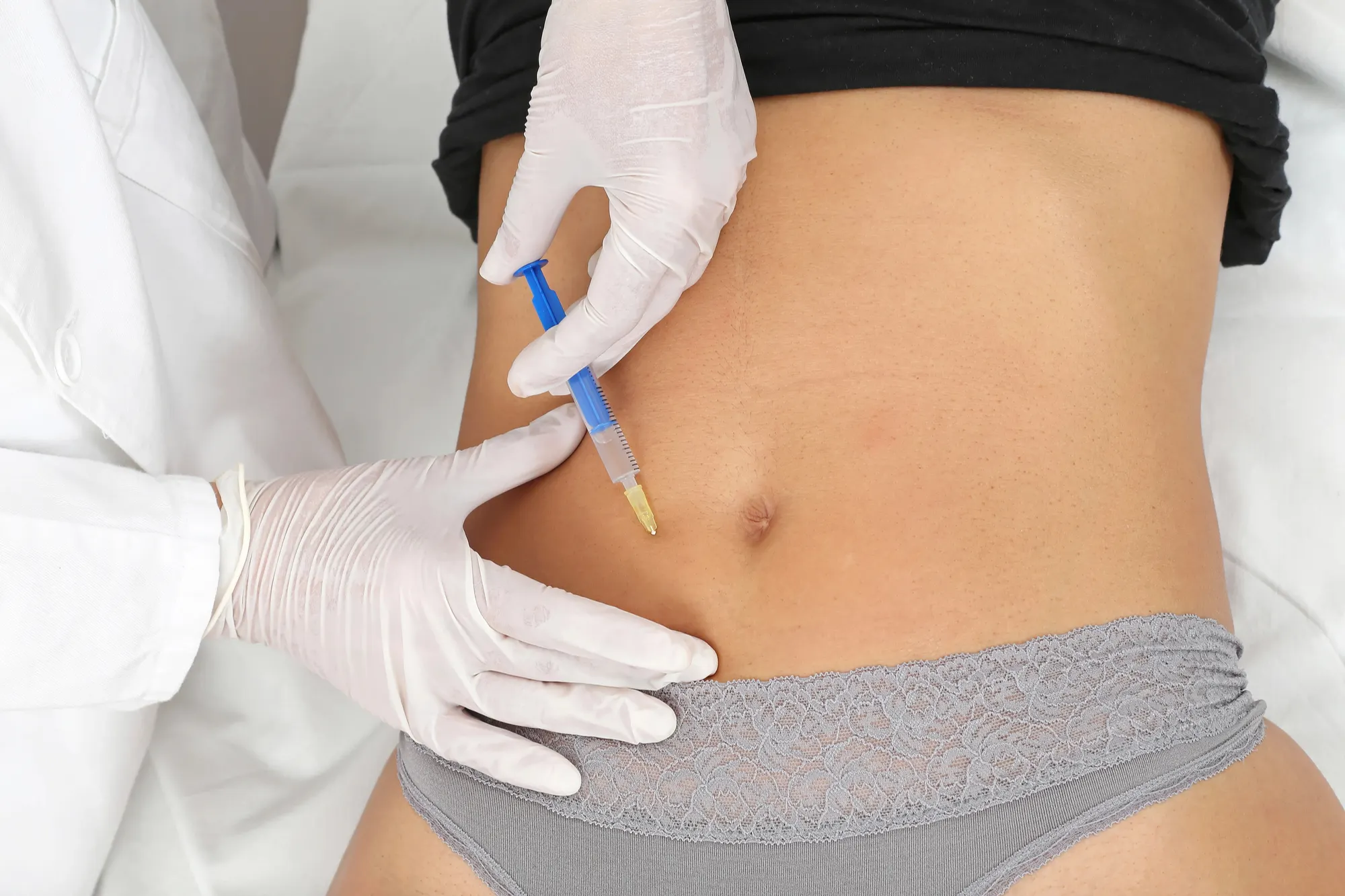
Administering the ‘Tummy BOTOX®’
The procedure typically begins with administering light propofol sedation to ensure patient comfort during the process. An endoscope is used to examine the stomach lining to rule out any abnormalities before proceeding.
Alternatively, some researchers have experimented with ultrasound guidance, using which BOTOX® is injected precisely into five specific locations in the lower stomach region, typically targeting the antral subserosa or muscularis propria approximately 2-3 cm above the pyloric ring.
These injections, performed under endoscopic control using a sclerotherapy injector needle, are strategically distributed around the gastric antral circumferences, starting at a distance of 3 cm from the pyloric ring.
Following the BOTOX® in stomach procedure, patients are closely monitored for two hours to detect any immediate side effects, and a follow-up phone call is made the next day for further assessment. Weekly weight measurements and repeated nutrient drink tests at 4 and 16 weeks post-procedure allow for ongoing evaluation of satiety and gastric function changes.
Meticulous documentation of injection details and patient responses enables the medical team to assess outcomes and ensure patient safety and efficacy of the procedure.
Are There Any Adverse Effects?
Although BOTOX® on stomach injections is generally well-tolerated, healthcare professionals should be aware of potential adverse events for patient counseling and management. Here’s a quick guide to the most common side effects:
Local Reactions
- Pain and tenderness
- Hematoma
Cutaneous Manifestation
- Rash, including erythema multiforme, urticaria, or psoriasiform eruptions.
- Pruritus
Allergic Reactions
- While uncommon, allergic reactions to botulinum toxin can occur. Symptoms include facial swelling, generalized urticaria, dyspnea, or dizziness.
Other Adverse Events
- Ptosis: Although more frequent with blepharospasm injections, ptosis is theoretically possible with gastric BOTOX® but is a rare complication.
- Temporary incontinence: Seen in a small percentage of patients treated for anal fissures in the form of transient incontinence of gas or stool. Alternative injection techniques or treatment modalities for patients with pre-existing fecal incontinence may be a better option.
- Pancreatitis: This is an extremely rare but potentially serious complication associated with botulinum toxin injections into the minor papilla.
- Antibody formation: Repeated or high-dose BOTOX® injections can lead to antibody development and potentially reduce treatment efficacy.
Here are some things healthcare professionals can integrate in their one-on-one consultations to mitigate the risk of untoward events
- Know the Side Effects: Understanding the spectrum of administering BOTOX® injection in stomach’s side effects allows for informed patient counseling and effective management.
- Select Patients Wisely: Meticulous patient selection based on medical history and risk factors.
- Communicate Clearly: Emphasize the transient nature of most side effects but discuss potential complications and encourage reporting unusual symptoms.
- Monitor Closely: Schedule follow-up appointments to monitor for adverse events and ensure prompt intervention if needed.
The Medication Way: Role of Weight Loss Drugs
When exploring alternatives to BOTOX® for the stomach to lose weight, there are various options beyond invasive procedures. Medications such as OZEMPIC® , SAXENDA®, and WEGOVY® offer non-surgical approaches to weight management, each with its own benefits and considerations.
- OZEMPIC® (Semaglutide): Originally approved for type 2 diabetes, Ozempic is a GLP-1 receptor agonist. It mimics a gut hormone to increase insulin release, decrease glucagon production, and delay stomach emptying, which contributes to weight loss.
- SAXENDA® (Liraglutide): Approved for chronic weight management, Saxenda, also a GLP-1 receptor agonist, works similarly to Ozempic. It regulates appetite, insulin, and digestion, to promote weight loss. Saxenda requires daily injections with a gradual dosage increase.
- WEGOVY® (Semaglutide): FDA-approved for weight management in obesity/overweight with comorbidities, offers higher doses than Ozempic. Studies show significant weight loss (up to 15% in 1.5 years).
Nevertheless, it is crucial to identify the optimal choice tailored to individual health status, treatment goals, and personal preferences. Also, potential side effects, cost implications, and drug availability hold weight when exploring alternatives.
Conclusion
While evidence suggests obesity treatments like stomach BOTOX® can benefit both physical and mental health, there is more left to uncover. Gastric BOTOX® procedure is a promising tool for weight loss, as supported by ongoing research. Its minimally invasive nature and ability to promote satiety hold significant potential for those seeking weight management solutions. However, choosing patients carefully is important, considering factors like BMI and prior weight loss response. To be most successful in the long run, gastric BOTOX® should be part of a bigger plan that includes healthy eating and exercise.
Advancements in technology tools like High-Resolution Manometry, Endoscopic delivery of BTX, improved imaging modalities, and Neurophysiological Studies have certainly contributed to our understanding of the effectiveness of BOTOX® in gastrointestinal disorders.
In addition, future research should tackle these limitations to grasp better how gastric BOTOX® influences a patient’s self-perception and mental state during weight management. Understanding these links is vital for improving obesity treatment and enhancing patient outcomes. Healthcare professionals can act as a bridge by staying abreast of the evolving research landscape in this field. By doing so, they can ensure patients the most effective and personalized treatments, leading to better results and better quality of life.
FAQ
1. Can you get BOTOX® on your stomach?
Yes, botulinum toxin (BOTOX® is a brand name) injections can be administered into the stomach wall to treat disorders affecting the abdomen. This procedure is also called gastric BOTOX® or endoscopic botulinum toxin injection.
2. Is stomach BOTOX® safe?
Generally, gastric BOTOX® procedure is considered safe when performed by a qualified healthcare professional. However, as with any medical procedure, there are potential risks and side effects. Discussing potential complications before going ahead with the procedure is essential.
3. What are the side effects of gastric BOTOX® injections?
Potential side effects of gastric BOTOX® include:
- Nausea
- Vomiting
- Indigestion
- Bloating
- Stomach pain
- Acid reflux
These are usually temporary and mild and require minimal intervention. More serious side effects are uncommon.
4. How effective is stomach BOTOX®?
Currently, studies show mixed results regarding the effectiveness of stomach/gastric BOTOX® for weight loss and other abdominal conditions. It may benefit some patients by helping them feel fuller for longer, leading to reduced calorie intake. However, it’s not a standalone solution and should be combined with diet and exercise for optimal results.
5. What is gastric BOTOX®?
Gastric BOTOX®, sometimes called stomach BOTOX®, is a non-surgical procedure for weight loss where botulinum toxin (BOTOX®) is injected into specific stomach regions via endoscopy. This aims to reduce stomach muscle contractions, delaying emptying and potentially inducing a feeling of increased satiety. It’s minimally invasive, with no surgical incisions, and patients can often resume normal activities on the same day. The effects usually last 4-6 months.
6. Is gastric BOTOX® FDA-approved?
At present, gastric BOTOX® is not FDA-approved for weight loss in the United States. However, it may be used off-label by some healthcare providers.
7. What can I eat after stomach BOTOX®?
Although there are no specific dietary restrictions after receiving stomach BOTOX® injections, it’s important to follow any specific dietary guidelines provided by your healthcare provider. Generally, you may be advised to start with clear liquids and gradually progress to soft foods before returning to your regular diet. It’s essential to avoid foods that could cause discomfort or exacerbate side effects during recovery. It’s generally recommended that you maintain a healthy, balanced diet and avoid excessive calorie intake to maximize weight loss benefits.
References
- Şen, O., & Türkçapar, A. G. (2020). Gastric Botulinum Toxin-A Application for Weight Loss Therapy. The Turkish Journal of Gastroenterology, 32(1), 66-69. https://doi.org/10.5152/tjg.2020.20076
- Lacy, B. E., Weiser, K., & Kennedy, A. (2008). Botulinum Toxin and Gastrointestinal Tract Disorders: Panacea, Placebo, or Pathway to the Future? Gastroenterology & Hepatology, 4(4), 283-295. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3093735/
- Mohajir, W.A., et al. (2023). Botulinum Toxin A Use in the Gastrointestinal Tract: A Reappraisal After Three Decades. Gastroenterol Hepatol, 19(4). Texas A&M College of Medicine and Baylor Scott & White Medical Center, Round Rock, Texas; University of Texas Health Science Center at Houston, Houston, Texas; University of Texas MD Anderson Cancer Center, Houston, Texas.
- Cardoso-Júnior, Aloísio & Savassi-Rocha, Paulo & Coelho, Luiz & Sposito, Maria & Albuquerque, Walton & Diniz, Marco & Paixao, Andre & Garcia, Frederico & Lasmar, Leonardo. (2006). Botulinum A Toxin Injected into the Gastric Wall for the Treatment of Class III Obesity: A Pilot Study. Obesity surgery. 16. 335-43. 10.1381/096089206776116408.