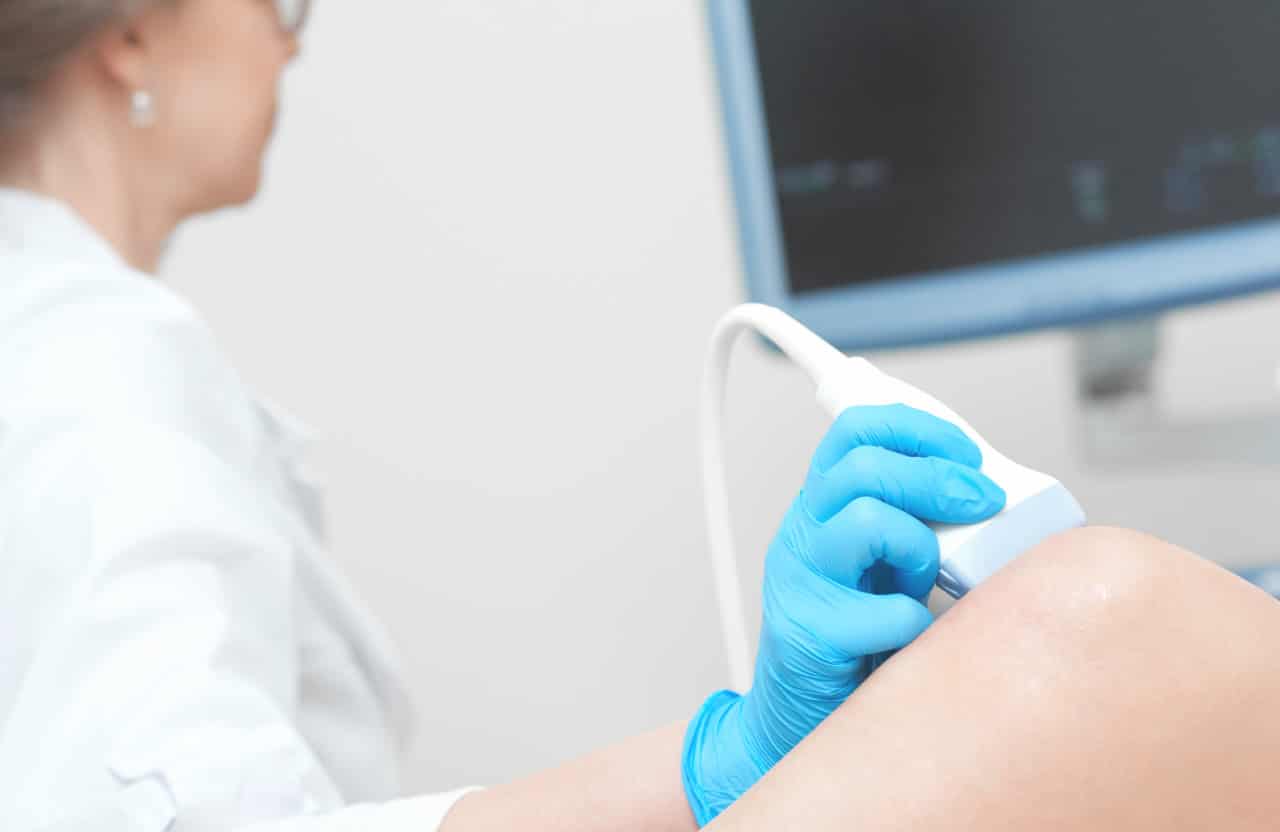
The need for extreme precision and safety in various medical procedures has led to the development of innovative techniques and their widespread adoption. Among these, ultrasound-guided injections are one of the most popular options.
The usage of ultrasound during injections enables healthcare providers to target specific tissues or structures with significant accuracy. This level of precision is particularly crucial in procedures involving delicate or deep-seated anatomical regions.
What Are Ultrasound-Guided Injections?
Ultrasound-guided injections, as the name suggests, are medical procedures that involve real-time ultrasound imaging to guide the precise placement of a needle or catheter into a specific anatomical target. This technique become popular over the years due to its potential to enhance accuracy and reduce complications.
The concept of utilizing ultrasound for medical imaging dates back to the early 20th century, but it was only in the mid-20th century that its practical application in guiding medical procedures began. Initially, ultrasound was primarily used for diagnostic purposes. However, its integration into therapeutic interventions, such as injections, has significantly expanded its utility in medical practice.
Ultrasound imaging provides real-time visualization of anatomical structures, soft tissues, and target areas within the body. This dynamic imaging capability allows healthcare professionals to navigate the needle or catheter to the desired location precisely, ensuring accurate placement and minimizing the risk of unintended tissue injury.
Using Ultrasound-Guided Injections
Performing ultrasound-guided injections necessitates specific equipment. The core of this procedure is the ultrasound machine, which provides high-frequency sound waves that create real-time images. Additionally, specialized needles or catheters equipped with echogenic markers enhance visibility during the procedure, aiding in precise needle placement.
Proper ultrasound-guided injection technique includes several steps:
- The first step involves locating the anatomical structure or target area of interest using ultrasound imaging. The high-resolution images generated by the ultrasound machine provide a clear view of the target, allowing the healthcare provider to plan the needle trajectory.
- With the target area identified, the healthcare provider carefully inserts the needle or catheter under real-time ultrasound guidance. Continuous monitoring of the ultrasound screen allows for precise needle advancement, ensuring that it reaches the intended location with minimal deviation.
- The operator monitors the needle position on the ultrasound screen throughout the procedure. Adjustments are made as necessary to ensure accurate placement, particularly in cases where the target is small or deep within the body.
While ultrasound-guided injections offer remarkable precision, certain technical tips can further enhance the success of the procedure:
- Opt for needles or catheters with enhanced visibility features, such as echogenic tips or shafts, to improve needle visualization during the procedure.
- Explain the procedure and provide reassurance, as patient comfort and relaxation will positively impact the success of the injection.
- Adequate training and experience in ultrasound-guided procedures are critical for the process. Providers should undergo comprehensive training to master the technique and understand the nuances of ultrasound-guided injections.
Benefits of Ultrasound-Guided Injections
Here is a list of proven ultrasound-guided injection benefits:
- Enhanced accuracy and precision. Unlike blind injections, where the anatomical target is inferred, ultrasound guidance provides real-time visualization, allowing doctors to visualize the needle’s trajectory directly and ensure it reaches the intended site with pinpoint accuracy.
- Reduced risk of complications and adverse effects. By visualizing nearby structures, vessels, and nerves in real-time, doctors can steer clear of critical areas, minimizing the potential for inadvertent injury or damage. This is particularly helpful in sensitive anatomical regions, such as nerve blocks, or when performing vascular access procedures.
- Enhanced patient comfort and satisfaction. Real-time imaging allows providers to avoid sensitive areas, resulting in a more comfortable experience. Patient comfort can lead to improved compliance and satisfaction with the procedure, contributing to a more positive procedure experience.
- Improved outcomes and quicker recovery. The precision guaranteed by using ultrasound for the injection procedure directly translates into improved clinical outcomes. Patients are more likely to experience the intended therapeutic effects of the treatment, whether it involves pain relief, improved joint function, or targeted medication delivery. Additionally, reduced trauma to surrounding tissues can lead to quicker recovery times, minimizing post-procedure discomfort and downtime.
Clinical Applications
Ultrasound-guided injections have found wide-ranging applications across several medical specialties:
- In orthopedics, ultrasound-guided injections help accurately deliver medications, such as corticosteroids or hyaluronic acid, into joints affected by osteoarthritis or inflammatory arthritis (for example, ultrasound-guided knee injection). Additionally, ultrasound guidance is invaluable for diagnostic aspirations and therapeutic interventions in cases of soft tissue lesions, such as ganglion cysts or calcific tendinitis.
- For pain management specialists, such injections can precisely deliver pain-relieving medications or anesthetics to targeted nerve roots, joint spaces (for example, ultrasound-guided hip injection), or soft tissue structures. Nerve blocks, facet joint injections, and epidural steroid injections are just a few examples of procedures enhanced by ultrasound guidance. Patients often experience faster and more effective pain relief, leading to improved quality of life.
- In rheumatology, ultrasound-guided injections have revolutionized the management of autoimmune and inflammatory joint diseases. By visualizing synovial inflammation and joint effusion in real time, rheumatologists can perform accurate joint aspirations and deliver medications directly to the affected site. This approach reduces disease activity and minimizes the systemic side effects of high-dose drugs.
- Gynecologists use this technique for various interventions, such as hysterosalpingography (HSG) to assess fallopian tube patency, endometrial biopsy for diagnosing abnormal uterine bleeding, and intrauterine device (IUD) placement. The real-time visualization provided by ultrasound ensures the safety and precision of these procedures, especially in the context of gynecological surgery.
The technique continues to evolve and find new applications across medical specialties, ultimately improving patient care and outcomes.
Side Effects and Contraindications
As with any medical procedure, careful patient selection is crucial when considering ultrasound-guided injections. While the technique offers numerous benefits, it may not suit all patients. Contraindications for the manipulation include:
- Patients with known allergies to medications or contrast agents;
- Active infections or local skin conditions at the injection site;
- Coagulopathy or bleeding disorders.
Patient cooperation and the ability to remain still during the procedure are essential for optimal outcomes. Individuals who cannot maintain the required position or remain calm may not be suitable candidates for ultrasound-guided injections.
While ultrasound-guided injections are generally considered safe and well-tolerated, certain side effects and potential complications may arise:
- Mild pain or discomfort at the injection zone, which usually subsides within a short period.
- Localized bruising or swelling at the injection zone.
- Although rare, infection at the injection area is a potential complication.
- There is a remote possibility of nerve injury in procedures involving nerve blocks. Careful patient selection, precise needle placement, and continuous monitoring during the process can reduce this risk.
- In vascular access procedures, such as central line placement, inadvertent vascular injury can occur. Real-time ultrasound guidance is instrumental in avoiding such complications.
Conclusion
Ultrasound-guided injections are a tool to use to provide unparalleled precision, reducing the chances of complications, and also offer enhanced patient comfort, improving clinical outcomes. The techniques described above have found applications throughout diverse medical specialties, certainly enhancing care delivery in orthopedics, pain management, rheumatology, obstetrics, gynecology, and beyond.
We encourage doctors to consider incorporating ultrasound guidance into their procedures, leveraging this technology to elevate the standard of care and improve patient outcomes.
FAQ
How painful is an ultrasound-guided injection?
The pain level experienced during an ultrasound-guided injection can vary from person to person and depends on several factors:
- Type of Injection. For example, some injections involve administering medications that may cause temporary discomfort, while others, like nerve blocks, may temporarily numb the area and reduce pain during the procedure.
- Patient pain thresholds and pain perception.
- The location of the injection.
- The skill and experience of the healthcare provider performing the procedure.
- The use of local anesthetics.
- Patient anxiety and fear of the procedure.
Doctors can minimize patient discomfort by using local anesthesia, precise needle placement, and open communication to ensure the patient’s well-being throughout the procedure.
What does an ultrasound-guided injection do?
An ultrasound-guided injection is a medical procedure involving real-time ultrasound imaging to guide the precise placement of a needle or catheter into a specific anatomical target within the body, for application of products such as Synvisc.
Ultrasound usage serves as a tool to enhance the precision, safety, and effectiveness of various medical procedures, allowing healthcare providers to directly visualize the target area, ensuring that therapeutic agents are administered where needed, ultimately improving patient outcomes and minimizing the risk of complications. The specific therapeutic goal of the injection will depend on the patient’s medical condition and the intended treatment or diagnosis.
How can a patient prepare for an ultrasound-guided injection?
Preparing for an ultrasound-guided injection involves several essential steps to ensure the procedure is safe and successful. Here’s a guide on how a patient can prepare:
- Inform the healthcare provider about their allergies and all medications they are currently taking, including over-the-counter drugs, supplements, and herbal remedies.
- On the day of the procedure, wear loose, comfortable clothing that can easily be adjusted to access the injection site.
- If sedation or anesthesia is used during the procedure, patients must arrange for a responsible adult to accompany them and drive them home following the injection.
References
Sahu AK, Rath P, Aggarwal BB. Ultrasound-guided injections in musculo-skeletal system – An overview. Journal of Clinical Orthopaedics and Trauma. 2019;10(4):669-673. doi:10.1016/j.jcot.2019.05.013.
Patel RP, McGill K, Motamedi D, Morgan T. Ultrasound-guided interventions of the upper extremity joints. Skeletal Radiol. 2023;52(5):897-909. doi:10.1007/s00256-022-04148-9.
Rastogi AK, Davis KW, Ross A, Rosas HG. Fundamentals of Joint Injection. AJR Am J Roentgenol. 2016;207(3):484-494. doi:10.2214/AJR.16.16243.
Lee RKL, Griffith JF. Top-Ten Tips for Ultrasound-Guided Joint Injection. Semin Musculoskelet Radiol. 2019;23(4):419-428. doi:10.1055/s-0039-1694755.