Injury implies that there is a need to restore a specific area and its structural integrity to normal function. It is an urgent need because mechanical integrity and the barriers are required to prevent any fluid loss or, even worse, severe infection. To reorganize the injured structure so that blood and lymphatic inflow and outflow is prevented is known as wound healing. Flawless repair is neither possible nor practical in the adult body, because of the aforementioned urgency. However, that is not to say that the other end of the spectrum does not exist. Regeneration is the term given to perfect and flawless repair without any scar formation, but it is only possible during the embryonic stage, and in certain tissues, such as the bone and liver. Unfortunately, the technology available today is unable to utilize this knowledge and put it into practical use. Interestingly, all wounds experience the same repair mechanisms. Acute wounds are repaired in an orderly and timely manner, while the repair of chronic wounds is stalled at various stages of the inflammatory process and fails to heal. In any case, scars tend to occur more often when the healing activity is disrupted, which is the case in most chronic wounds. Factors such as increasing age, cardiac or renal failure, location on the body, atherosclerosis, amount of tissue damaged, and foreign material embedded can affect the development of scar formation. These scars can be a major hindrance for many patients to achieve their ideal look. As such, this article will focus mainly on the types of treatment available for the variety of scars that an individual can suffer from.
Types of scars
In general, there are five types of scars: normal mature scars, immature scars, hypertrophic scars, keloids, and atrophic scars. Not all of these scars may need to be considered for treatment. the Hypertrophic and keloid scars are commonly described synonymously, as both represent a similar concept: they are scars raised from the normal skin contour and may be itchy and painful. One key difference is that keloid scars are found extending outwards out of the normal tissue boundary, while hypertrophic scars are confined in the boundaries.
Scar treatments
From the cosmetic standpoint, plastic surgeons and dermatologists can offer a multitude of treatment techniques or methods to treat scars, depending on the type of scar. For example, steroid injections are used on hypertrophic and keloid scars, as they can help shrink them, whereas surgery is used to modify the scar. The list of treatments elaborated below do not represent an exhaustive list, but they are intended to help guide you on the treatment options.
Topical treatments
The key with any treatment modality is that it has to be evidence-based. Most topical treatments for scars remain controversial to this day, as the current scientific literature on these modalities provides limited evidence for their use. For example, take Vitamin E. It has been used worldwide as an anti-scarring agent. In theory, Vitamin E is an active component that has antioxidant properties to help reduce the severity of a scar. This theory was further bolstered by anecdotal reports that supported this use, but clinical studies later refuted this theory and instead reported increased incidences of adverse effects. As of now, there exists minimal evidence to support the use of Vitamin E to minimize scarring. More research is vital and must precede vitamin E use by patients.
Another popular option is onion extracts. They work by decreasing inflammation and reducing the fibroblast proliferation rate, the latter of which reduces collagen deposition. Despite this encouraging mechanism of action, clinical studies on postsurgical scars were not well received. The beneficial findings from these studies are small-scale, not randomized or double-blinded. Their quality of evidence is poor. There exists no solid evidence to develop any recommendations concerning their use for scars.
Chemical peels
Chemexfoliation are mainly used on atrophic scars that are left by acne vulgaris. The chemical injury induced can remodel the collagen deposition and lead to a better aesthetic outcome. Examples of chemical peeling agents are trichloroacetic acid, salicylic acid, glycolic acid, Jessner’s solution, and phenol. For optimal results, they are usually done concurrently with microneedling and laser. 4 There is no universal standard as to how these combination treatments can be used, which has led to many differing treatment regimens.
Corticosteroid injections
Injectable steroids are known to decrease scarring through reducing inflammation and fibroblast growth and subsequent collagen synthesis, causing vasoconstriction that limits wound oxygenation and nutrition, which in turns influences transforming growth factor-beta 1 and 2 and collagen in keratinocytes. Injectable steroids also increase collagen degeneration. A widely used corticosteroid is triamcinolone. The use of triamcinolone is further supported by a few studies; the patients in these studies had reported efficacy rates of 50 to 100%, but they also had recurrence rates of 9 to 50%. Side effects such as dermal atrophy and hypopigmentation can also occur with the use of these injections. Regardless, its benefits outweigh the risks for most patients, and due to this, it is mostly recommended as a first-line therapy for hypertrophic and keloid scars. These injections must be administered intralesionally, as topical corticosteroids have little to no effect on the scars.
Silicone sheets
Silicone sheets are commonly bought and used for hypertrophy scar prophylaxis and treatment. The use of these sheets is supported by the 2001 International Advisory Panel for Hypertrophic Scarring and Keloid Management, which stated that this treatment modality is a viable option in view of other effective treatment modalities. Also, many plastic surgeons have advocated for the use of these products as well. Their mechanism of action is thought to arise from their temperature, oxygen tension, and hydration regulation. However, despite the overwhelming support from the aesthetic community, the clinical studies that support its use are considered to be of poor quality and highly prone to bias. The popularity of this treatment modality may instead stem from its cost effectiveness, availability, non-invasive nature, and the possibility that it may improve scars. A further recommendation of this treatment modality, however, requires more conclusive studies.
Dermal fillers
Injectable dermal fillers are versatile treatment methods that can be used for indications other than scars. They offer excellent and quick results for patients with atrophic scars, such as infamous “ice pick” scars. They can be used alongside with surgical subcision so as to produce better results, as they can work together synergistically. The needle used to inject one of these fillers can be inserted below the scar tissue, where the filler material is to be deposited. Filling of this particular space causes the surface of the scar to rise so that the natural contours of the body is restored. Filler materials include hyaluronic acid and calcium hydroxyapatite.
Microneedling
Microneedling is considered a minimally invasive technique and involves the use of a surgical tool with multiple needles. There are a wide variety of devices for microneedling use, such as manual rollers with needles from 0.5 to 3mm and a stamping battery-powered device. The needles penetrate the skin at a uniform depth at the dermis layer. This results in a skin injury that is controlled to a certain degree. The injury induces wound repair by way of collagen and elastin deposition. The outcome is improved skin texture and firmness with an overall increase in skin quality. The scars are also reduced to a significant degree. Microneedling has been used for other purposes than treating scars, such as reducing pore size and cellulite. Microneedling does not require any anesthesia, and for the best improvements, multiple sessions need to be conducted.
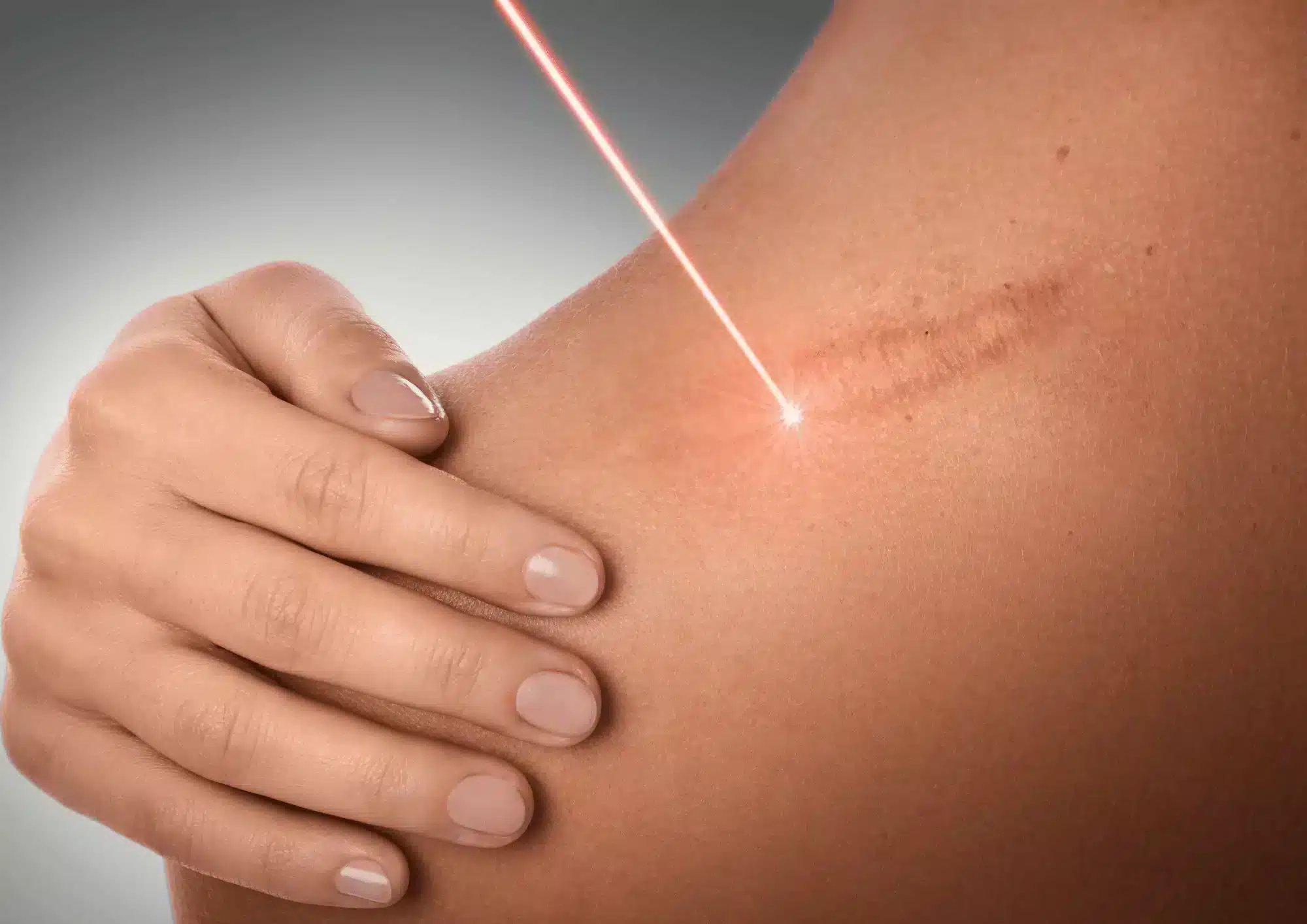
Lasers
Lasers are specialized devices used for prophylaxis and also for restructuring hypertrophic and keloid scars. In the earliest revisions, ablative, nonselective lasers were using carbon dioxide or erbium yttrium aluminum garnet. The carbon dioxide variant caused wound contraction, induced collagen remodeling, activated fibroblast growth factor, and reduced transforming growth factor beta. The latter variant induced a heat shock response to influence the levels of transforming growth factor beta. Though the theory behind the use of either is sound, neither saw much use due to the adverse reactions they caused. They were known to cause significant burn injuries, which meant that the risks were too overwhelming to recommend them. Later on, the development of pulsed-dye laser and laser-assisted skin healing laser meant better patient tolerance and more satisfactory results. A review done in 2010 found that both of these provide excellent clinical results on scar volume, texture, and erythema. Following another review, it was determined that the 595-nm type laser consistently offers better efficacy than its 585-nm counterpart. Regardless, keloid scars are known to recur with the use of the laser modality, and their recurrence rate has been described as rapid in some cases of treatment with a pulsed laser. A combination of a laser with either intralesional steroids or 5-fluorouracil may offer better results. Fractional lasers and intense pulsed light, on the other hand, are newer advancements in the scene. Non-ablative fractional lasers have a stronger safety profile and are more efficacious than ablative lasers. Fractional lasers are known to work by inducing thermal injury and epidermal necrosis at thermal zones where that are separated by areas of normal tissue. These normal tissues can help in the healing process by migrating to the damaged sites. However, there is currently very limited evidence supporting the use of non-ablative lasers.
Case study: hypertrophic scar treatment
Platelet rich plasma (PRP) is another available treatment method designed for treating scars. PRP is used because it can improve the wound healing process. The discussion regarding platelet rich plasma will be continued through a case study.
Patient A, who is a 36-year-old female, is an airline pilot that has a history of cervical discectomy that dates back to October 2015. The initial injury was caused when she overreached for a control in the deck, which then resulted in the paralysis of the arm. Post-surgery, she recovered and developed an aesthetically acceptable paramedian scar at the anterior side of the neck on the left. Four months after the incident, the wound started to undergo hypertrophy. She went for treatment for the scar in April 2016, and it was diagnosed as a hypertrophic scar. Prior, she also had two papillomas over the scapula that was removed before the incident.
The removal had also resulted in hypertrophic scars that were treated with steroid injections but to no avail. Based on this information, she was counseled to use PRP for the neck scar. She was informed that steroid injections may cause further thinning of the skin and uneven skin tone, while PRP can help strengthen the wound and reduce the scar’s appearance. Laser therapy was considered, but the wound was too confined for a chance of a successful outcome. Other treatments, such as topical creams and chem-exfoliation, were similarly abandoned. PRP was believed to be the best treatment option for this patient taking into account the obvious scar location.
PRP
Growth factors, present in platelet rich plasma, are excellently suited for scar tissue remodeling (e.g. vascular endothelial growth factor, basic fibroblast growth factor, and platelet derived growth factor). PRP, as a treatment, is ideal for soft and bony tissue repair; trials are being conducted to determine effectiveness on new and matured scars. PRP is collected via centrifuged autologous blood, through purpose-made PRP kits. The process for administration is simple and straight forward: directly injecting at the intra-dermal or sub-dermal level.
PRP has been in the market for about five decades ago, and its first high profile use was in an open-heart surgery that was done in Italy in 1987. As research continues, the indications for PRP grow wider into other treatment areas. Nowadays, PRP can be used for leg ulcers, gum recession, and even genital rejuvenation.
Treatment
Prior to administering PRP, a thorough medical history was obtained to make sure none of its contraindications, such as coagulopathies, warfarin use, non-steroidal anti-inflammatory drug use, and an existing infection, were present She was informed on the transient side effects that are common with injections, such as erythema, edema, and infection. After that, treatment started with 20ml of drawn whole blood with an anticoagulant. This blood was then centrifuged and the plasma activated via calcium, both of which produced 8ml of active PRP. The scar was then deposited with multiple 0.2ml PRP aliquots. 1ml of PRP was also deposited at the deep dermis level.
Review
First, post-treatment follow-up was done after eight weeks. The scar significantly improved with an overall decrease in erythema except from the borders, which remained as before. It was also noted that the scar was flatter except for the outer side areas. She remained optimistic that the scar can still see further improvements in terms of color and shape. She also maintained that her daily routine is affected, as she found it strenuous to conceal the scar without a scarf. She underwent a second PRP procedure, and she was again reviewed in eight weeks. Subsequently, the imperfections of the previous treatment were resolved. The scar no longer looked erythematous, and the entirety of the scar seemed to have flattened out. She was booked for a follow-up six months after so as to again review her condition.
The future
The future is exciting, as more novel therapies are being pushed down the line. One such advanced treatment method is the plasma beam therapy. It is capable of delivering curved beams of plasma energy that are produced by charged gases (i.e. room air). Such a treatment modality is also portable via machines called Plasma IQ or Plexr. Significant advances include its non-invasive nature and its ability to be used without anesthetic. It is ideal for upper blepharoplasty and also for most types of scars.
References
1. Kokoska M, ‘Hypertrophic Scarring and Keloids’, Medscape (2016) <http://emedicine.medscape.com/ article/876214-overview>
2. Baumann LS, Spencer J, ‘The effects of topical vitamin E on the cosmetic appearance of scars’, Dermatol Surg, 25(1999) pp.311-5.
3. Vitamin E, Evidence (US: Mayo Clinic, 2016) <http://www.mayoclinic.org/drugs-supplements/vitamin-e/ evidence/hrb-20060476>
4. M. C. Annunziata, V. D’Arco, V. De Vita, G. Lodi, M. C. Mauriello, F. Pastore, and G. Monfrecola, ‘Acne Scars: Pathogenesis, Classification and Treatment. Gabriella Fabbrocini’,Dermatol Res Pract, 2010.
5. S Kokoska, MD & Arlen D Meyers, Hypertrophic Scarring and Keloids Mimi, (2016) <http://emedicine. medscape.com/article/876214-overview#a1>
6. Juckett G, Hartman-Adams H, Management of Keloids and Hypertrophic Scars’, Am Fam Physician, 80(2009) pp.253-260.
7. Neerja Puri and Ashutosh Talwar J, ‘The Efficacy of Silicone Gel for the Treatment of Hypertrophic Scars and Keloids’, Cutan Aesthet Surg, 2(2009) pp.104106.
8. Orentreich N, ‘Subcutaneous incisionless (subcision) surgery for the correction of depressed scars and wrinkles’, Dermatol Surg, 21(1995) pp.543-9.
9. Jesitus J, Collagen-stimulating fillers provide rejuvenating advantages, naturally (US: Dermatology Times, 2012) http://www.dermatologytimes.modernmedicine.com/dermatology-times/news/ modernmedicine/modern-medicine-feature-articles/collagen-stimulating-fillers-?page=full
10. Moers-Carpi M, Vogt S, Santos BM, et al. Dermatol Surg. 2007;33 Suppl 2:S144-S151
11. Lewis W, ‘Is microneedling really the next big thing?’ Plastic Surgery Practice, 7(2014) pp.24-28
12. Liebl H, Kloth L, ‘Skin cell profliferation stimulated by microneedles’, J Am Coll Clin Wound Spec https:// www.ncbi.nlm.nih.gov/pmc/articles/PMC3921236
13. Ngan V, Fractional laser treatment (New Zealand: DermNet New Zealand, 2015) http://www. dermnetnz.org/topics/fractional-laser-treatment/
14. Dalton M, Treating vascular lesions (US: The Dermatologist, 2013) http://www.the-dermatologist.com/ content/treating-vascular-lesions/
15. Rui Jin, Xiaolu Huang, Hua Li, Yuwen Yuan, Bin Li, Chen Cheng, Qingfeng Li, ‘Laser Therapy for Prevention and Treatment of Pathologic Excessive Scars’, Plastic and Reconstructive Surgery, 231(2013).
16. Coondoo A, ‘Side-effects of topical steroids: a long overdue revisit’, Indian Dermatol Online J, https:// www.ncbi.nlm.nih.gov/pmc/articles/PMC4228634
17. Jean L Bolognia, Joseph J Jorizzo, Julie V Schaffer, Dermatology, (2012) p.2262.
18. Textor J, ‘Platlet-Rich Plasma (PRP) as a Therapeutic Agent: platelet biology, growth factors and a review of the literature’, Springer.
19. Parrett BM, Donelan MB, ‘Pulsed dye laser in burn scars: current concepts and future directions’, Burns., 36(4) (2010), pp.443-9.
20. Hu MS, Zielins ER, Longaker MT, Lorenz HP. Scar prevention, treatment, and revision. (ed). Plastic Surgery: Volume 1: Principles, 4th ed. : Elsevier; 2018. pp. 196-213.
21. Tziotzios C, Profyris C, Sterling J. Cutaneous scarring: Pathophysiology, molecular mechanisms, and scar reduction therapeutics. Journal of the American Academy of Dermatology 2012; 66(1). https://www.clinicalkey.com/#!/content/journal/1-s2.0-S019096221101067X?scrollTo=%23top (accessed 27 July 2018).