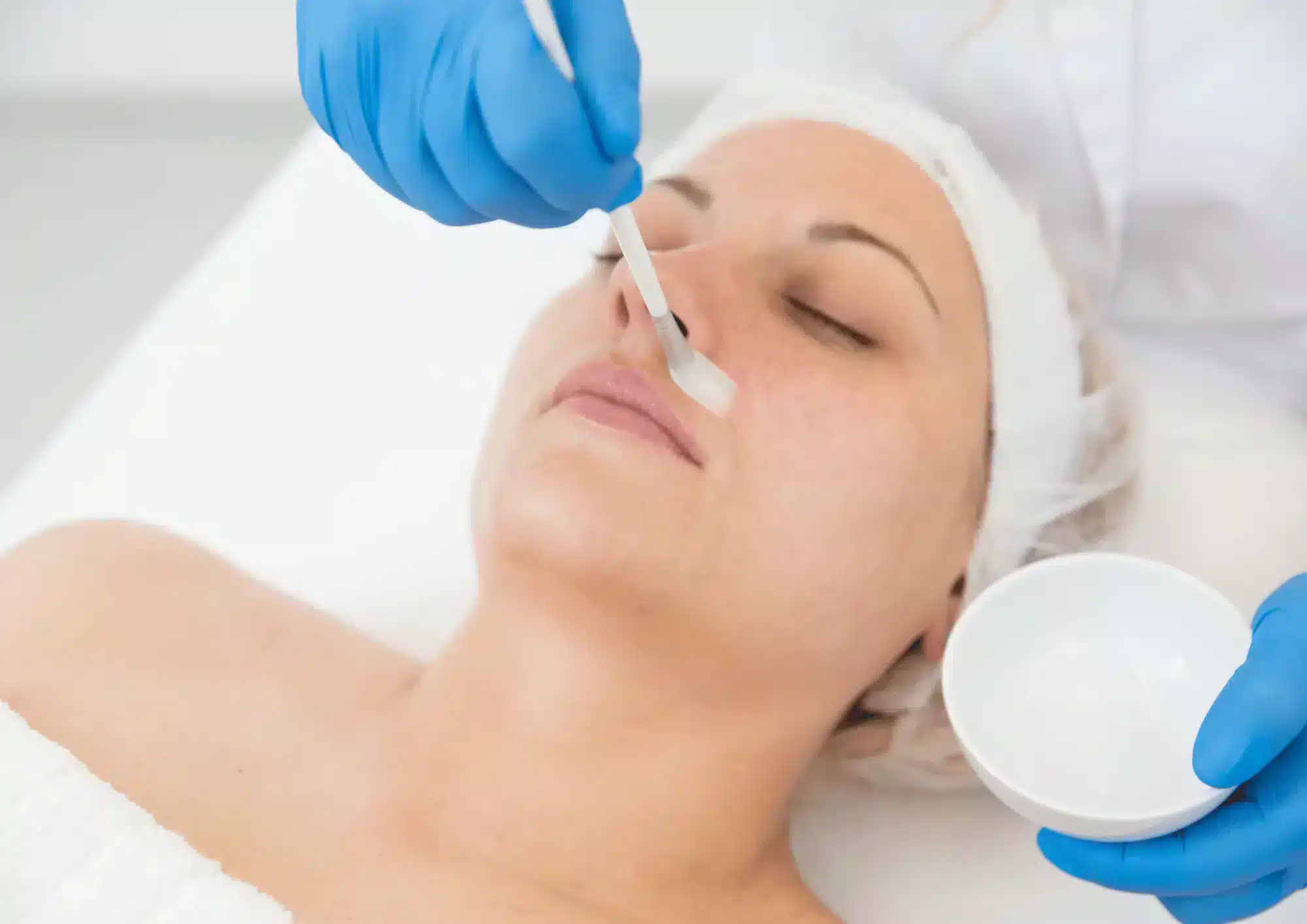
Chemical peels are aesthetic treatments aimed at conditioning the skin of the face or body. These treatments involve the use of a chemical solution that incurs controlled destruction at a specific skin depth, resulting in the sloughing off of dead skin. Once this occurs, newly regenerated skin replaces the old layer, which is usually smoother and has less pigmentation and blemishes. Chemical peeling has been practised in the field of dermatology since the early 1950s, when phenol was used to treat acne scarring. These preliminary techniques have since evolved with time and have given rise to the use of other aviable peeling agents, such as trichloroacetic acid (TCA) and alpha hydroxy acids (AHAs) that penetrate the skin at different depths to produce different results. This produces an improved side effect profile and a shortened recovery period.The chemical peel is a common treatment in aesthetic practices due to its efficacy in treating the signs of aging such as dull skin, discoloration, wrinkles, and loss of skin elasticity. As such, it is important for practitioners to have a comprehensive understanding of the different types of chemical peels, their mechanisms of action, expected results and potential complications, as well as cautions and contraindications and interactions with other products like Ellanse, in order to select the correct treatment for each patient. Given the wide selection of peels available, selecting the appropriate peel treatment is not always easy and can be confusing, especially for non-dermatologists. This only strengthens the need for more research and training on the correct and proper use of chemical peels.
Identifying and preparing chemical peels
Chemical peels are grouped by depth of penetration and severity of injury. Superficial peels penetrate to any depth within the epidermis to the stratum basale, whereas medium-depth peels act deeper to the papillary dermis, and deep peels have the deepest activity, down to the level of the reticular dermis. Superficial peels can be further divided into very superficial and superficial peels, with very superficial peels having activity only down to the stratum corneum.
The depth of peel is not necessarily determined by the peeling solution. Peel depth relies on other variables as well, including the concentration of the solution, pH level of the solution, availability of free acid, skin condition, method of application, and the length of time applied to the skin. For instance, a glycolic acid 70% solution may act as a superficial peel if only left on the skin for five minutes but can cause the effect of a medium depth peel when applied for 15 minutes.
An emerging trend in chemical peel treatment is the combined peel approach, where different agents are used one after another for a synergistic effect. This approach also has the added benefit of a reduced side effect profile. Examples include applying Jessner’s TCA and a 70% glycolic acid peel prior to 35% TCA.
Prior to a chemical peel, it is standard practise to have the patient undergo a regimen of skin preparation to minimize the risk of undesired effects, such as post-inflammatory hyperpigmentation (PIH); to anticipate any potential issues with products used during or after the procedure; and to maximize the benefits and achieve optimal rejuvenation. Such regimens will usually include some combination of a low concentration alpha hydroxy acid cleanser or moisturizer, a product with retinol of isotretinoin, and a skin-lightening agent such as hydroquinone or kojic acid. As well, the regimen should include an SPF product to help reduce melanocyte excitability. Ideally, the regime should be implemented for a minimum of two weeks prior to peeling.
What are medium peels?
Medium depth chemical peels, known simply as medium peels, are used in the treatment of fine lines and wrinkles that result from photoaging, and in pigmentary disorders and minor atrophic scars. The classic agent used in medium peels is TCA in concentrations of 40–60%. This concentration range, while effective, poses a higher risk of complications like pigmentation and scarring. These days, medium peels have a lowered TCA concentration of 35% in combination with other ingredients, usually Jessner’s, 70% glycolic acid or solid carbon dioxide. These treatments are as effective as treatment with 50% TCA but produce fewer risks.
TCA, the medium depth peeling agent of choice, is a protein denaturant. It is a water soluble agent that is not able to penetrate easily into the sebaceous skin, which is rich in lipids, which is why skin has to be preconditioned and superficial peels applied first before applying TCA, so that the stratum corneum is increased in permeability and any surface oils on the skin are removed. This will result in a deep and even penetration of TCA, for a more even and consistent depth of protein denaturation..
Glycolic acid 70% and 35% TCA
This combination peel approach produces the same effects as the Jessner’s technique but finds an alternative superficial peeling agent in glycolic acid. Glycolic acid is a keratinolytic agent and permits greater penetration of 35% TCA. It is usually applied for two minutes before it is neutralized with a bicarbonate solution or cold water. Glycolic acid is not suitable for dry or inflamed areas of skin, as the decreased skin barrier in these areas may inadvertently cause 70% glycolic acid to penetrate deeper than intended.
Jessner’s solution and 35% TCA
Jessner’s solution contains salicylic acid (14g), lactic acid (14g) and resorcinol (14g) and is made to 100 ml with ethanol. This peel is applied for keratinolytic purposes, to alter the permeability of the epidermal barrier to allow for the TCA solution to penetrate more rapidly and more evenly.2 Before applying this solution, the skin is cleansed and exfoliated with acetone to remove sweat and sebum. Any hypertrophic actinic keratoses may be subject to curettage at this stage. The peel is applied to the skin using a cotton applicator until a layer of speckled white frost and uniform erythema is attained. Once the desired endpoint has been achieved, any burning or discomfort can be eased with cool water compresses. After washing off the solution, applying a topical anaesthetic like available EMLA creams or LMX can help enhance the comfort of the patient.
After washing off the numbing cream and drying the skin, 35% TCA is then applied to the skin in an even layer using cotton-tipped applicators or small gauze swabs. Once application has resulted in a uniform layer of white frosting and background erythema is seen, cool compresses can be applied to soothe the burning sensation. The sensation should last about 10 minutes before subsiding. After the burning sensation has dissipated, an occlusive ointment (for example, Aquaphor or Vaseline) can be applied to reduce post-treatment dryness.
Solid carbon dioxide and 35% TCA
This approach uses an acetone-coated solid block of carbon dioxide that is applied to the skin to create injury to the epidermal region. The depth of injury incurred is dependent on the time of application, and depth of penetration and peel of the subsequently applied TCA solution. With this in mind, areas that need deeper peeling, like moderate wrinkles, scarring and thick actinic keratosis, can be pre-treated with a longer application of solid carbon dioxide for better results. This technique potentially affords greater aesthetic improvement; however, results are greatly dependent on the skill and technique of the operator.
What to expect
Right after treatment, the patient may experience some swelling and tightness in the skin. However, these symptoms can be managed with continuous application of occlusive ointments a few times a day. This is important because shortened recovery times and less incidence of persisting redness will be beneficial to the patient. By the third day, the epidermis above the level of chemical injury will separate from the underlying skin. With this, serious exudate and crusting are to be expected. This separation of the skin usually starts from the perioral area, and spreads to the whole face from there, with the forehead peeling last. During this time, the patient should not pick at the shedding epidermis, as scarring could occur. However, any hanging dead skin can be trimmed off with sharp scissors. The patient can apply a moisturizer five days after skin exfoliation begins, and the peeling process may continue for 10 days more. After this process is done, the new skin that emerges is usually noticeably more even and brighter in tone. Any pigmentation and blemishes should be improved in appearance, and fine lines and wrinkles are diminished. Further improvement in results will be maintained through the ongoing process of dermal remodelling, resulting in neocollagenesis after around six weeks. Depending on the skin condition, more peels may be recommended to sustain the revitalization. After three weeks, the patient’s pretreatment skincare regimen can resume.
What are deep peels
Most of the literature concerning deep peels is centred on the use of phenol. While TCA at concentrations of greater than 50% has been used, the associated incidence of adverse events make phenol a preferable alternative.
Phenol has a similar mode of action to TCA in that it works by penetrating through the dermis to cause denaturation and coagulation of proteins at a particular dermal depth. However, phenol penetrates the skin more rapidly down to the reticular dermis. For this reason, phenol peels are characterized as a quick peel. This means the there is less room for adjustment in terms of depth than that of TCA.
Phenol has been used as a peeling agent over the past decades in a variety of formulations. It was first used as a medium depth agent at a concentration of 88% (undiluted). This was adjusted further in the Baker-Gordon formula, which combines phenol with septisol soap, croton oil, and water to allow for a deeper penetrative effect than pure phenol alone. Further modifications to this formula were described by Stone and Venner-Kellson, which entailed altering the croton oil concentration and adding olive oil and glycerine. Any of these preparations will give the same outcome, as long as reticular dermis protein coagulation is attained.
Deep peeling is indicated for moderate to severe wrinkles, acne scars, and dyschromias. Deep peeling will have a better effect on wrinkles and pigmentation than medium depth peels, as the epidermolysis is complete and involves the papillary dermis, something that cannot be achieved by medium depth peels.
Phenol deep peeling
Phenol peels can be uncomfortable for the patient. Due to this reason, sometimes they are given anesthesia. At the bare minimum, a choice of oral or intravenous sedation should be available pre-, intra-, and post-operatively. For this treatment, the skin is prepared in the same manner as for a medium depth peel, resulting in clean and degreased skin. The phenol solution is then applied to the skin using rolled and rung gauzes to each facial section. Once an individual section has been treated, the solution is washed off and treatment then proceeds for the subsequent area. The endpoint for this treatment is determined as a frost of grey-white coagulated protein, with loss of erythema within the frosting indicating that the peel has progressed beyond the vascular loops of the papillary dermis.
An important issue to consider when using a deep phenol peel is the higher risk for severe complications. Not only is there a higher incidence of scarring, PIH, hypopigmentation, and delayed healing, the phenol itself is systemically absorbed and is cardiotoxic, and thus carries the risk of heart failure. Risk of a cardiac event is dependent on the volume of phenol used; therefore, any full-face treatment is undertaken in sections, completing one area before moving on to the next. Cardiac monitoring in an appropriate clinical environment is highly recommended for this type of treatment. As well, antiviral and antibiotic cover is necessary throughout the treatment, and the patient is usually prescribed oral steroids.
What to expect
Recovering from a deep phenol peel takes longer and is more involved than medium peeling. For the first 48 hours after treatment, an occlusive dressing, such as a waterproof tape mask, is needed. The skin is exudative and wet, requiring careful wound care with applications of thymol iodide several times daily for one week. In the first week, movements of the mouth can crack the developing wound in the perioral area, so patients are advised to limit mouth movements by consuming a blended diet through a straw. By day nine, a new epithelial layer should have formed, and the dead peel mask can be debrided gently with regular warm compresses and emollient applications. The new skin will be red and swollen and may remain in that condition for up to four weeks. The results of a phenol peel are impactful and long-lasting, with dramatic improvements in facial wrinkles, skin texture, and pigmentation.
Avoiding complications
Treatments with chemical peels are regarded as very effective. However, there are complications associated with them. Some patients carry factors that make them at-risk for developing complications and should be excluded from treatment. Risk factors include cigarette smoking, immunocompromised status, poorly controlled diabetes, a history of recent or current herpes simplex infections, recent facelift or laser resurfacing, and a history of hypertrophic and/or keloid scarring. A history of isotretinoin use should also be specified, as use within the preceding six to 12 months may increase the likelihood of scarring.
For medium-depth chemical peels, the most common effect is erythema, which should fade within three to four weeks. Occasionally, erythema may be prolonged, and could be an indicator of sensitized skin, compounded by prior skin disease such as eczema or rosacea, or caused by unintended deeper peel depth. A rarer effect of medium depth peels is scarring. This may occur several months after treatment and can be projected early by discerning areas of prolonged and intense erythema and induration. Scarring can be avoided or lessened with early and prompt topical steroid treatment. Patients with a history of herpetic lesions may find recurrence or development of herpetic lesions, which is also common in other patients. For this reason, a history of herpetic lesions should be specifically enquired about when taking down the patient history, and antiviral prophylaxis should be prescribed to patients who are at risk. In fact, some doctors prescribe antiviral medication routinely to all patients undergoing chemical peels.
Infections, although rare, should be identified early due to magnified symptoms (pustules, greater than expected erythema, excessive crusting and more intense pain) in patients in the recovery period. Swabs for mycology, bacteriology, and virology should be taken and, following lab results, appropriate empirical treatment commenced. Permanent hypo-pigmentation is a side effect that is expected to occur with higher incidence in dark-skinned individuals after deeper peels. Hypo-pigmentation is also associated with complications like infection during the recovery period. As well, PIH is also a potential complication, and can be managed with appropriate pre-treatment preparation and with topical application of 4% hydroquinone, should it occur.
In short, prudent patient selection, appropriate choice of peel, pretreatment and close observation of endpoints should all reduce the rates of occurrence of complications.
Screening patients
The medical history of the patient will be helpful at this point to guide the treatment course. Some patients may not be suitable for deeper peels, due to risk factors like hepatic and renal impairment, history of scarring, previous surgery or radiation treatment, or history of cardiac events, in the case of phenol treatment. The patient seeking a chemical peel treatment should also be made aware of the high degree of pre and post-treatment wound care that is necessary for successful outcomes. Patients who may not be as willing to undergo a prolonged period of recovery may consider a chemical peel treatment of lesser depth that is repeated more frequently (for instance, a medium depth peel repeated every six months to one year would be preferable to a single deep peel). As well, the patient should consider the risk-benefit profile of the treatment they are looking at in order to justify the higher risk versus greater outcome.
Chemical peel treatments should ideally address the patient’s concerns and utilize the full extent of treatment options available to the practitioner. During initial consultation, a thorough assessment of the patient’s skin type and degree of photoaging should be the top priority. For this, two assessment scales that are pertinent are the Glogau scale of photoaging, which measures the extent of photoaging damage and thus indicates the appropriate peel type; and the Fitzpatrick classification of skin type, which groups skin types by color and reaction to sun exposure, and therefore gives insight into the likelihood of PIH, hypopigmentation, and scarring.
Finally, the last issue the patient should consider when selecting a chemical peel treatment is the choice of practitioner. The outcome of these procedures relies upon the skill, technique and experience of the practitioner: an experienced practitioner is more likely to get a better result than a beginner. Accordingly, a practitioner who is just starting out with chemical peels should make every effort to gain a comprehensive understanding of skin anatomy and physiology, as well as the modes of action of the various chemical peels available, they should also get experience in performing the procedure under an experienced practitioner’s supervision.