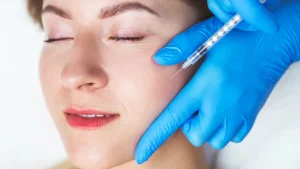
Patients with facial hyperhidrosis, which is excessive sweating of the face, are often embarrassed by their condition. For these patients, social and occupational situations can cause great anxiety and hamper their lifestyle. Many of the standard modalities used to treat hyperhidrosis may offer only limited success, as is the case with many topical antiperspirants, such as endoscopic transthoracic sympathectomy or tap water iontophoresis, which are not applicable for use in the facial area. Fortunately for these patients, Botox may be a viable treatment option. In this article, the role of Botox in the management of facial hyperhidrosis will be discussed.
Facial hyperhidrosis, and how Botox treats it
Facial hyperhidrosis is a type of focal hyperhidrosis, a condition where sweat is produced to an amount that exceeds physiological needs. In general, facial hyperhidrosis is bilateral and primarily affects the forehead. In some cases, other facial regions—such as the scalp, temples, nose, chin, neck, and cheeks—may also be involved. Facial hyperhidrosis falls into four distinct pattern types: ophiasis (the most common pattern), upper lip, diffuse or whole scalp, and Frey syndrome. This condition can be diagnosed using the Minor starch-iodine test, where the level of sweating is evaluated through the observation of color changes in areas applied with iodine and corn starch; the presence of sweat will cause the yellow iodine to turn dark blue.
Botox is indicated for primary axilla hyperhidrosis and is routinely used to treat other types of focal hyperhidrosis, including plantar and palmar hyperhidrosis. It acts to reduce the activity of the sweat glands via chemical denervation. Botox acts on the nerve endings within the treatment area to prevent the release of acetylcholine, a neurotransmitter that essentially gives muscles the signal to contract, so disrupting the transmission of this signalling to the sweat glands will partially paralyze them and consequently reduce sweat production.
Botox treatment for hyperhidrosis is very effective, with results that last, at a minimum, for five months. One study showed that 90% of patients who received Botox treatment for this indication were satisfied with their results. Its widespread cosmetic use in a myriad of other indications is also a testament to its safety and tolerability profile.
The treatment procedure
Carrying out this procedure without causing undesired side effects, such as muscle weakness and pain, requires a high degree of expertise on the part of the medical practitioner. To make the treatment more comfortable for the patient, a topical numbing cream may be applied prior to the injection procedure.
The standard dilution recommended for cosmetic use, which is 2.5ml of 0.9% preservative-free saline per vial, can be applied for a Botox treatment of facial hyperhidrosis. In general, this volume is sufficient to cover the treatment area, but larger volumes of the Botox solution may be required if the scalp is treated as well. The total dose used for treatment will vary by area of treatment. If treating the forehead alone, a total dose of 40 units is typically used. These 40 units should be injected in a series of 20–30 injections that are spaced approximately 2cm apart from each other, so as to ensure overlapping Botox halos for sufficient coverage. Due to the fact that patterns of facial hyperhidrosis greatly vary on a case-by-case basis, there is no standard injection grid for treatment. To avoid the diffusion of Botox into the underlying muscles, the dose per site should not exceed five units.
While it is preferable to inject Botox into non-hair bearing skin, injection into the scalp may be required in some cases. When planning the injection grid, avoid the caudal strip 1–2cm above the eyes: injecting in this area may cause the drooping of the eyelid. If the treatment of the cheeks is necessary, it is important to plan the injection sites carefully due to the potential for aesthetic alterations in facial expressions to occur. In a similar vein, caution should also be exercised when treating the entire craniofacial area, including the back of the neck, in order to avoid the risk of neck weakness.
The injection procedure should be carried out with a 30-gauge needle. Botox should be injected into the deep dermis at or close to the dermal-subcutaneous junction. Because the injections may cause the extrusion of the Botox solution, it is recommended to inject this solution at an oblique angle of approximately 45°, so as to create a longer injection track. Skin blanching with injection indicates the correct placement of the drug.
After treatment, the patient should be observed in a clinical setting for 30 minutes to monitor for adverse reactions to the Botox. It is also recommended that the practitioners follow up on their patients roughly two weeks after the procedure to verify if the treatment is working for them.
Potential side effects of Botox treatment for facial hyperhidrosis
The main concern with using Botox to treat facial hyperhidrosis is the risk of it causing aesthetic side effects, such as brow ptosis or facial asymmetry. Additionally, brow asymmetry is another potential side effect; if this occurs, it is usually temporary, typically only lasting a few weeks, and will resolve spontaneously. Minor muscle weakness has also been reported in certain cases; this weakness usually manifests itself as an inability of the afflicted patient to frown or furrow their forehead. That being said, the treatment is considered safe and rarely causes adverse effects. The best way to reduce the risk of unwanted effects is to ensure your injector is licensed and experienced.
Conclusion
Facial hyperhydrosis is known to cause certain regular issues—from hindrances of daily activities such as sweat dripping into the eyes, or from anxiety connected to one’s appearance—for afflicted patients. These issues, very quickly, can in a negative way affect anybody’s psychological and emotional state. Thankfully, Botox has been created to prevent exactly these same infuriating, and possibly debilitating issues from occurring. This is due to Botox being an effective method of managing facial hyperhydrosis in a semi-permanent, minimally invasive manner.