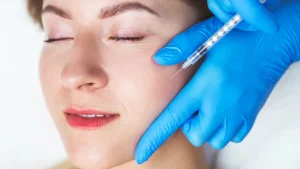
Introduction
The use of dermal fillers, particularly hyaluronic acid (HA)-based fillers, has become the predominant standard for non-surgical treatment of aging skin. HA fillers have surpassed collagen as the most popular cosmetic filler. Producing minimal side effects, having a reversible nature, and lacking immunogenicity, this option is preferred by practitioners and patients alike.
As with any cosmetic procedure, the outcome of this treatment largely depends on the physician’s skill and knowledge, rather than the filler itself. The demand for safe, long-lasting, and biocompatible dermal fillers continues, as a growing number of individuals prefer minimally invasive treatments for cosmetic procedures.
Pre-procedure care
It cannot be stressed enough that dermal filler injections must only be performed by trained and licensed medical professionals. Aside from having the appropriate credentials, the administrator must have a comprehensive knowledge of the process of aging and concomitant skin conditions, the types of fillers available, and the appropriate injection techniques.
Patient Assessment
It is the responsibility of the physician to determine the appropriateness of any requested procedure. There are many factors to consider before the appropriate treatment plan can be devised for a patient. Some patients will have unrealistic expectations of their results, which should be addressed early on.
Prior to treatment:
• Assess the patient’s psyche;
• Obtain a thorough medical history of the patient;
• Consider the desired outcome of the patient;
• Assess the area with the patient in an upright position;
• Take pretreatment photographs for study;
• And identify the injection sites using washable marker.
Filler Selection
Reversible or temporary fillers are recommended for patients who are unfamiliar with dermal filler injections. Appropriate fillers depend on the defect to be corrected, the type of material used, and the longevity desired. HA fillers do not require allergy testing, while collagen-based fillers are of bovine origin, and as such must be pretested prior to administration.
Intra-Procedure Care
Cleansing
On the day of treatment, patients should remove any cosmetics from their face and wash it with mild soap. Patients must sit in an upright position in a comfortable chair. The area will be prepared for filler injection following strict aseptic techniques.
Anesthetizing
The type of anesthesia required depends on the area to be treated, as well as the patient’s pain threshold. To reduce discomfort, topical anesthesia may be applied 30 to 60 minutes prior to the procedure. Topical anesthetics include lidocaine and tetracaine, in various combinations. There are also a wide variety of fillers pre-mixed with lidocaine.
For physicians – injection
The physician must be aware of the right injection techniques used for each filler, and site where they will be deposited. Unwanted effects, such as overcorrection, can be remedied by injecting the enzyme hyaluronidase (for hyaluronic acid-based fillers) into the skin.
During the procedure:
• Adhere to correct depth of injection;
• Correct product label or batch number sticker on consent forms;
• And document the procedure by indicating the filler used, quantity, and areas treated.
|
Common Injection Methods |
Indication |
Technique |
| Threading Method | Used for treating the vermillion border | Involves depositing the product as the needle is withdrawn from the tissue |
| Serial Droplet Method | For treating glabellar lines and periorbital hollows | Commonly used for silicone injection |
| Fanning Method | For nasolabial folds | The preferred method for superior, natural, and longer lasting results. Needle is passed back and forth under the fold, depositing the filler as the needle is inserted and withdrawn |
Post-Procedure Care
After the procedure is complete, the treated area will be cleaned, and markings will be removed using alcohol, hydrogen peroxide, or a similar antiseptic solution. Ensure you follow all instructions for aftercare methods as provided by the injector.